5 Ways to Calm Menopause Reflux (From Someone Who Gets It)
I remember the night I sat straight up in bed at 2 a.m., convinced something was seriously wrong. That burning sensation crawling up my chest? Turns out it wasn’t a heart attack. It was menopause reflux and nobody had warned me it was coming.
If you’re in your 40s or 50s and suddenly dealing with heartburn that seems to appear out of nowhere, you are not imagining it. The hormonal shifts of perimenopause and menopause genuinely change how your digestive system works. And for those of us already managing gut issues like IBS or bloating during menopause, it can feel like a real double whammy.
The good news? There are real, actionable things you can do about it. Let’s dig in.

Key Takeaways
- Declining estrogen weakens the lower esophageal sphincter, making menopause reflux more common.
- Smaller, more frequent meals are one of the fastest dietary shifts you can make to reduce symptoms.
- Trigger foods and lifestyle habits (like late-night snacking) matter more than ever during midlife.
- Probiotics, phytoestrogen-rich foods, and stress reduction can support your gut-hormone connection naturally.
- Sleep position and quality directly impact how much acid escapes at night and how rested you feel.
Why Menopause Reflux Happens in the First Place
Before we get to solutions, let’s talk about the why because understanding your body makes the fixes actually stick.
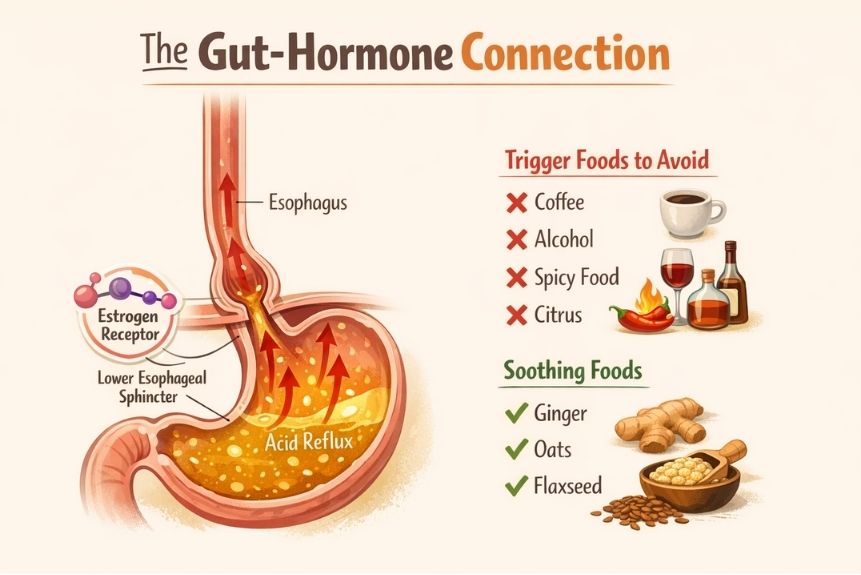
Your lower esophageal sphincter (LES) is basically a valve between your esophagus and stomach. It’s supposed to stay closed so stomach acid doesn’t creep upward. But here’s the thing: that valve has estrogen receptors [1]. When estrogen levels drop during menopause, the LES weakens and becomes less reliable at keeping acid where it belongs [1].
Add in slower gut motility, meaning food moves through your digestive system more sluggishly, and you’ve got a recipe for midlife digestive flare-ups.
💬 “Think of your LES like a screen door with a broken spring. It used to snap shut automatically. Now it just… hangs there.”
This is also connected to the broader gut-hormone connection and something called the estrobolome, the specific group of gut bacteria responsible for metabolizing estrogen. When your microbiome diversity drops (which it does during menopause), your estrobolome becomes less effective, and hormonal imbalance can worsen digestive issues.
Now let’s fix it.
1. Rethink How (and When) You Eat to Ease Menopause Reflux

This one sounds almost too simple, but the size and timing of your meals make a massive difference for menopause reflux.
Large meals require more stomach acid to digest. More acid means more opportunity for that weakened LES to let some escape upward. The fix? Eat smaller amounts, more often [1].
Try this approach:
- Aim for 4–5 smaller meals throughout the day instead of 3 large ones.
- Stop eating at least 3 hours before bed. Lying down with a full stomach is basically an invitation for reflux.
- Eat slowly. Rushing through meals causes you to swallow air, which increases bloating and pressure on the LES.
- Avoid eating past 7 p.m. if nighttime reflux is your main complaint.
Common menopause reflux trigger foods to reduce or avoid:

I personally had to say a very tearful goodbye to my morning espresso. I replaced it with ginger tea, and honestly? My gut thanked me within a week.
2. Move Your Body to Reduce Menopause Reflux (But Time It Right)
Regular movement is one of the most underrated tools for managing hormonal gut health during menopause.
Exercise reduces cortisol: the stress hormone that, when chronically elevated, actually increases acid production [2]. It also supports healthy gut motility (that’s just a fancy word for how efficiently food moves through your digestive tract) and helps with the weight management piece.
Here’s the important caveat: Timing matters.
- Don’t exercise right after eating. Wait at least 90 minutes.
- Avoid high-impact workouts (running, jumping) if you’re mid-flare. These can jostle acid upward.
- Do prioritize: walking after meals, gentle yoga, swimming, or cycling.
Research also shows that losing just 5–10% of body weight can significantly reduce reflux symptoms [1]. Hormonal changes during menopause make weight management harder, but even gentle, consistent movement makes a real difference over time.
Stress reduction is part of this too. Mindfulness practices like meditation, deep breathing, and yoga lower cortisol and reduce acid production [2]. Even 10 minutes of slow breathing before bed can help.
3. Support Your Gut-Hormone Connection With the Right Foods and Supplements
Understanding the gut-hormone connection changed everything for me. Your gut bacteria don’t just digest food, they help regulate estrogen levels through the estrobolome. When your microbiome is out of balance, everything from bloating to reflux gets worse.
Phytoestrogen-rich foods are a natural, evidence-based way to gently support estrogen balance [1]:
- Flaxseeds: Add a tablespoon to oatmeal or smoothies daily.
- Edamame and tofu: Great dairy-free protein sources.
- Tempeh: Fermented soy that also supports microbiome diversity.
- Chickpeas and lentils: Affordable, versatile, gut-friendly.
If you’re dealing with lactose sensitivity in menopause (extremely common, by the way, as dairy digestion often worsens as estrogen drops), cutting out dairy can reduce both reflux and bloating significantly. This is a core part of bio-individual nutrition: what worked for your body at 35 may not work at 52.
On supplements:
- Probiotics containing multiple bacterial strains have been shown to improve reflux, bloating, constipation, and stress-related gut symptoms in menopausal women [2]. I’ve tested quite a few, so you can check out my roundup of the best probiotics for menopause bloating for my current top picks.
- Vitamin E (400 IU daily) has been studied in menopausal women and linked to fewer hot flashes and reduced reflux episodes [1].
- Black cohosh showed a 25% reduction in hot flashes in studies involving over 1,400 women, with reflux improvements often following [1].
⚠️ One important note: If you’re on or considering hormone replacement therapy (HRT), talk to your doctor about reflux specifically. Counterintuitively, research shows HRT can actually increase GERD risk in estrogen-only therapy by as much as 41% [1]. This doesn’t mean HRT is wrong for you, but it’s worth knowing.
Also, limit NSAIDs like ibuprofen whenever possible. They irritate the stomach lining and make reflux worse [3].
For a soothing, gut-friendly meal that checks a lot of these boxes, try my turmeric broth detox soup. It’s one of my go-to recipes during a flare.
4. Apply Low-FODMAP Principles to Manage Menopause Reflux Triggers
Not all “healthy” foods are reflux-friendly. Some high-fiber or fermentable foods can worsen bloating and pressure on the LES, especially during perimenopause bloating relief mode.
Low-FODMAP for midlife isn’t about restriction forever. It’s about identifying your specific triggers through a temporary elimination phase, then reintroducing foods systematically.
Gut-friendly, low-FODMAP foods that tend to be reflux-safe:
- Oats, rice, and quinoa
- Cooked carrots, zucchini, and green beans
- Bananas and melons (in moderation)
- Lean proteins: chicken, turkey, fish, eggs
- Ginger and turmeric (both anti-inflammatory)
- Bone broth (gut-healing and soothing. See my bone broth recipe for women in menopause)
Foods that seem healthy but can worsen reflux:
- Raw onions and garlic (high FODMAP, LES-relaxing)
- Tomatoes and tomato-based sauces
- Mint (yes, even “soothing” peppermint tea can relax the LES)
- Carbonated drinks
The goal isn’t perfection. It’s pattern recognition. Keep a simple food-symptom journal for two weeks and you’ll start seeing your personal triggers clearly.
5. Optimize Your Sleep to Break the Nighttime Reflux Cycle

Nighttime reflux is its own special kind of misery. You finally fall asleep, and then the burn starts. Cough. Wide awake at 3 a.m.
Adequate, restorative sleep helps keep cortisol levels lower, which directly supports GERD management [3]. But reflux also disrupts sleep. It’s a frustrating cycle. Here’s how to break it:
Practical nighttime strategies:
- Elevate the head of your bed by 6–8 inches. A wedge pillow works well and is less disruptive than raising the whole bed frame.
- Sleep on your left side. This positioning keeps the stomach below the esophagus and reduces acid exposure.
- Don’t eat within 3 hours of bedtime (yes, I’m saying it again because it matters that much).
- Wear loose clothing to bed. Tight waistbands increase abdominal pressure and push acid upward.
- Limit alcohol in the evening. Even one glass of wine can relax the LES and trigger nighttime symptoms.
A Quick Reference: Your Menopause Reflux Action Plan
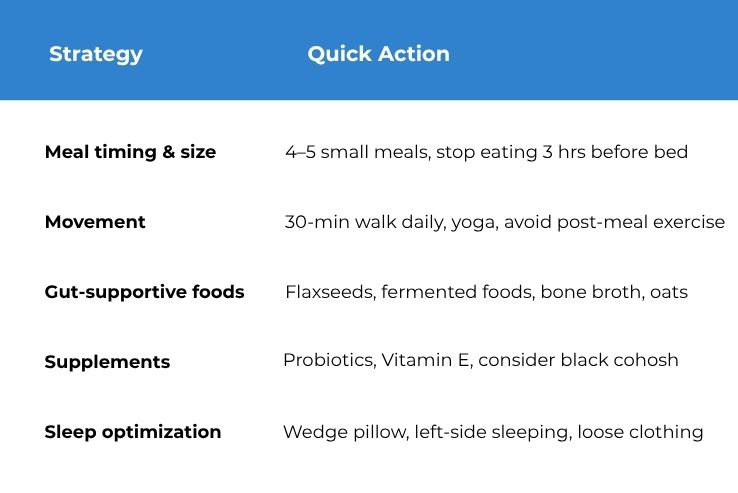
Conclusion: You Don’t Have to White-Knuckle Through This
Menopause reflux is real, it’s common, and it’s connected to the same hormonal shifts affecting everything else in your body right now. But it’s also highly manageable with the right combination of dietary shifts, movement, gut support, and smarter sleep habits.
Start with one change this week. Just one.
My recommendation: Begin with meal timing. Stop eating three hours before bed tonight and see how you feel tomorrow morning. That single shift has made the biggest difference for me personally.
From there, layer in the other strategies one at a time. Your gut doesn’t need a dramatic overhaul, it needs consistent, compassionate attention.
You’ve got this. And I’m right here navigating it alongside you. 💛
Trial and error is okay. Giving up is not.
XOXO,



Ready to Fast-Track Your Relief?
If you’re feeling overwhelmed by where to start, or if your IBS and menopause bloating feel like they need a dedicated “intervention,” I’ve created something specifically for you.
I’ve taken everything I’ve learned from my own journey and the science behind Better Belly Co. to create “The Better Belly Reset: 7 Days to De-Bloat and Restart Your Digestion.“
Inside this FREE PLAN, I’ll show you:
- The exact 7-day meal plan designed to be gentle on the gut and high in bloat-busting minerals.
- The “Better Belly” List: A belly-friendly grocery guide focused on low-FODMAP, high-mineral foods.
- The “Gut-Hormone” morning ritual to kickstart motility before your first cup of coffee.
Click here to download The Better Belly Reset for free and let’s get you back to feeling like yourself again.
You’ve got this. We’ve got this. And I’ll be with you every step of the 7-day way.
References
[1] Menopause And Acid Reflux – https://goldmanlaboratories.com/blogs/blog/menopause-and-acid-reflux
[2] What Causes Heartburn During Menopause And What Can You Do – https://thebettermenopause.com/blogs/the-better-gut-community/what-causes-heartburn-during-menopause-and-what-can-you-do
[3] Menopause And Gerd – https://www.henryford.com/blog/2024/04/menopause-and-gerd
Note about Safety:
Note: These statements have not been evaluated by the FDA. These products are not intended to diagnose, treat, cure, or prevent any disease. Always consult your healthcare provider before starting any new supplement, especially if you have existing health conditions.

Jacqueline Ramirez
I help women in perimenopause and menopause navigate gut health with clarity and confidence. Through simple, gut‑safe food systems and real‑life guidance, I make eating feel calmer and more manageable again.






