5 Signs your Gut is Changing During Menopause
Disclosure: This post contains affiliate links. If you purchase through these links, I earn a small commission at no extra cost to you. I only recommend products I’ve personally researched and trust.
Let me tell you something that nobody warned me about when I hit my late 40s: my gut decided to stage a full-blown rebellion right alongside my hormones.
One day I’m managing my IBS-C with my usual routine, and the next? My belly looks six months pregnant by 3 PM, foods I’ve eaten for decades suddenly betray me, and I’m Googling “digestive issues and menopause” at 2 AM because I can’t believe this is actually happening.
Here’s the truth: you’re not imagining it, and you’re definitely not alone.
A groundbreaking 2025 study presented at The Menopause Society’s Annual Meeting revealed that a staggering 94% of perimenopausal and menopausal women experience digestive health symptoms[1]. Even more telling? 82% of us reported that these symptoms either started or got significantly worse during the menopause transition[1].
This isn’t just “getting older.” This is your gut-hormone connection going through a major renovation and nobody gave you the blueprint.

Key Takeaways
- 94% of women in perimenopause and menopause experience digestive symptoms, with 82% reporting onset or worsening during this transition[1]
- Declining estrogen directly impacts your gut microbiome, reducing diversity and slowing gut motility. The “why” behind that stubborn bloating and constipation
- The estrobolome (gut bacteria that process estrogen) becomes less efficient during menopause, creating a vicious cycle of hormonal and digestive imbalance
- New food sensitivities aren’t random. They’re linked to shifts in your microbiome composition and reduced digestive enzyme production
- Professional support often falls short: 58% of women who sought help found it inadequate, making bio-individual nutrition and self-advocacy crucial[1]

Sign #1: The 3 PM Bloat That Won’t Quit (Even When You’re “Eating Clean”)
You know this scenario all too well. You start the day feeling relatively normal, maybe even optimistic. By mid-afternoon, you’re unbuttoning your jeans under your desk and wondering if you accidentally swallowed a beach ball.
Welcome to the most common sign of digestive issues and menopause: relentless bloating and gas.
In that same 2025 study, 77% of perimenopausal and menopausal women reported increased bloating or gas after meals[1]. That’s more than three out of four of us dealing with this daily frustration.
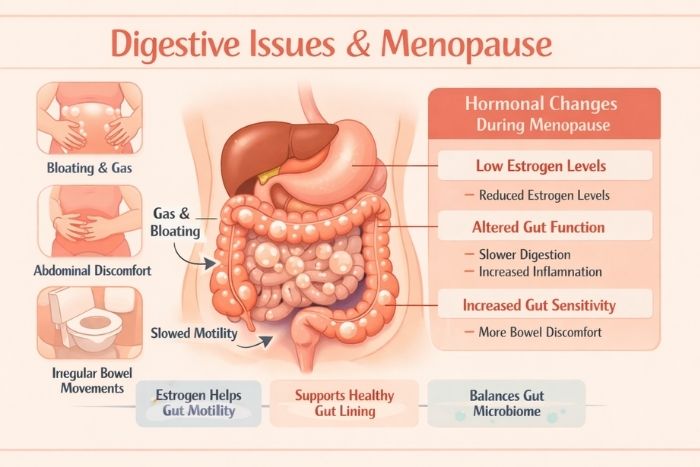
Why This Happens: The Estrogen-Gut Connection
Here’s what’s really going on behind the scenes. Estrogen isn’t just about reproduction. It plays a massive role in maintaining your microbiome diversity and keeping your digestive system running smoothly[2].
When estrogen levels start their perimenopausal roller coaster (and eventually decline), your gut microbiome actually shifts to resemble a pattern more commonly seen in men[2]. I’m not kidding.
This shift means:
- Less microbial diversity (fewer beneficial bacteria doing their jobs)
- Increased gas production from bacterial imbalances
- Reduced ability to break down certain foods
- More water retention in your intestinal tract
What You Can Actually Do About It
Stop blaming yourself first. This isn’t about “eating clean” or having more willpower. This is hormonal gut health in action.
Try these actionable steps:
- Track your bloating patterns for two weeks. Note when it happens, what you ate, and where you are in your cycle (if you still have one). Patterns reveal triggers.
- Eat your largest meal earlier in the day when your digestive fire is strongest. Gut motility naturally slows as the day progresses, and menopause makes this worse.
- Consider a low-FODMAP approach for 2-4 weeks to identify specific trigger foods. This isn’t forever. It’s detective work. (More on this article to why menopause bloating and IBS-C happen)
- Support your microbiome diversity with prebiotic foods like cooked and cooled potatoes, asparagus, and garlic (if tolerated)
I personally found that my afternoon bloating improved significantly when I moved my protein-heavy meal to lunch and kept dinner lighter. This is where bio-individual nutrition becomes your best friend.
Sign #2: Constipation Becomes Your Unwelcome New Normal
If you’re suddenly dealing with constipation or what I call “the mystery of the disappearing bowel movements,” you’re in abundant company.
54% of women in the menopause study reported constipation or irregular bowel movements[1]. That’s more than half of us struggling with what should be a basic bodily function.
And here’s the kicker: 50% also reported abdominal discomfort or cramping, often with that frustrating sense of incomplete emptying[1]. You know that feeling: you go, but you don’t really go.
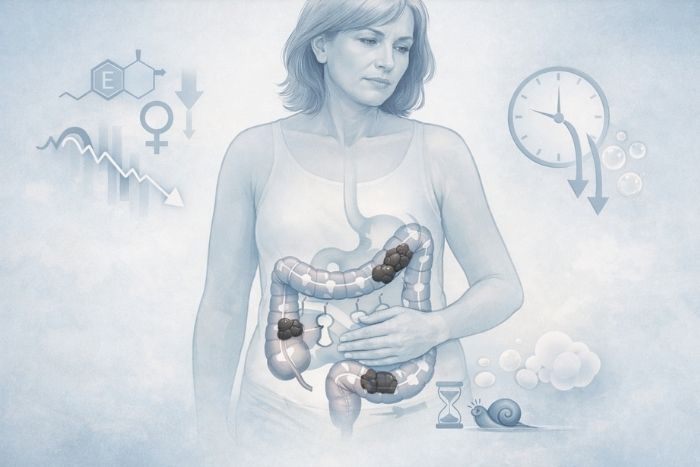
The Science Behind Slower Gut Motility
Both estrogen and progesterone influence how quickly food moves through your digestive tract. When these hormones decline during perimenopause and menopause, your gut motility slows down significantly[1][2].
Think of gut motility like a conveyor belt in a factory. When it’s moving at the right speed, products (waste) move through efficiently. When it slows down, everything backs up, gets stuck, and creates a traffic jam.
This slower transit time means:
- Stool sits in your colon longer, becoming harder and drier
- More water gets reabsorbed from waste (making it even harder to pass)
- Beneficial bacteria have less diverse material to work with
- You feel bloated, uncomfortable, and frankly, miserable
For those of us already managing IBS-C, this is the double whammy I mentioned. Our constipation-predominant IBS gets turbocharged by hormonal changes.
Practical Relief for Midlife Constipation
First, let’s talk about what doesn’t work: ignoring it and hoping it resolves itself. Trust me, I tried that approach for six months.
What actually helps:
- Hydrate strategically—aim for half your body weight in ounces of water daily, and front-load it in the morning. Consider adding electrolyte powders designed for women in menopause to improve absorption.
- Move your body daily, even if it’s just a 15-minute walk after meals. Movement stimulates gut motility naturally.
- Prioritize magnesium-rich foods like pumpkin seeds, spinach, and dark chocolate (yes, really). Magnesium glycinate supplements can also help without the harsh effects of magnesium oxide.
- Establish a morning routine that includes warm liquids (I swear by my morning gut-healing bone broth or warm lemon water) and 10 minutes of unrushed bathroom time.
- Consider a quality probiotic specifically formulated for constipation relief—check out my tested probiotic recommendations for bloating
The goal isn’t perfection. It’s consistency. Literally.
Sign #3: Foods You’ve Eaten Forever Suddenly Become Enemies
This one really got me. I’d been managing my lactose intolerance for years with a pretty predictable list of safe foods. Then perimenopause hit, and suddenly my “safe” list started shrinking.
Eggs? Bloating. Almonds? Gas. Even certain vegetables that never bothered me before started causing midlife digestive flare-ups that left me feeling defeated and confused.
You’re not losing your mind—you’re experiencing the reality of shifting food sensitivities during menopause.
Why Your Gut Suddenly Hates Everything
Here’s what’s happening at the microscopic level. Your gut microbiome composition changes during menopause, and not in a good way[3].
The estrobolome: that specialized group of gut bacteria responsible for metabolizing estrogen becomes less efficient as estrogen levels decline.
This creates a feedback loop:
- Less estrogen → Less diverse microbiome
- Less diverse microbiome → Poorer estrogen metabolism
- Poorer estrogen metabolism → Even more hormonal imbalance
- More hormonal imbalance → More digestive chaos
Additionally, your production of digestive enzymes decreases with age and hormonal changes. This means foods that you previously broke down efficiently now sit in your gut partially digested, feeding the wrong bacteria and creating gas, bloating, and discomfort.
The Lactose Sensitivity Plot Twist
For those of us already managing lactose intolerance, menopause can intensify our sensitivity or cause it to develop for the first time.
I’ve noticed my lactose threshold (the tiny amount I could sometimes tolerate) basically disappeared during perimenopause. Even trace amounts in processed foods now trigger symptoms.
Why this happens:
- Declining estrogen affects the intestinal lining
- Reduced enzyme production (including lactase)
- Increased gut permeability (“leaky gut”)
- Changes in gut bacteria that normally help digest dairy
Navigate New Food Sensitivities Like a Detective
Stop playing food roulette and start gathering data:
- Keep a detailed food and symptom journal for at least three weeks. Note everything you eat, how you feel 2-4 hours later, and your stress levels. Patterns will emerge.
- Try an elimination approach with common midlife triggers: dairy (obviously), gluten, high-FODMAP foods, caffeine, and alcohol. Remove them for 3-4 weeks, then reintroduce one at a time.
- Embrace bio-individual nutrition: Check what works for your best friend might be terrible for you. This is about your unique gut-hormone connection, not a one-size-fits-all diet.
- Focus on gut-healing foods like bone broth, cooked vegetables, fermented foods (if tolerated), and anti-inflammatory fats like olive oil and avocado.
- Work with a functional nutritionist who understands the intersection of digestive issues and menopause. The 2025 study found that 58% of women felt their professional support was inadequate[1]. Find someone who actually gets it.
Remember: These food sensitivities aren’t necessarily permanent. As you support your microbiome diversity and manage hormonal changes, some foods may become tolerable again.
Sign #4: Heartburn and Acid Reflux Crash the Party
If you’ve suddenly developed heartburn or acid reflux during perimenopause or menopause, you’re experiencing one of the most underreported digestive issues of this transition.
49% of women in the 2025 study reported heartburn and acid reflux[1]. But here’s the statistic that really caught my attention: post-menopausal women are almost three times more likely to have GERD symptoms compared to pre-menopausal women[1][3].
Three times more likely. Let that sink in.
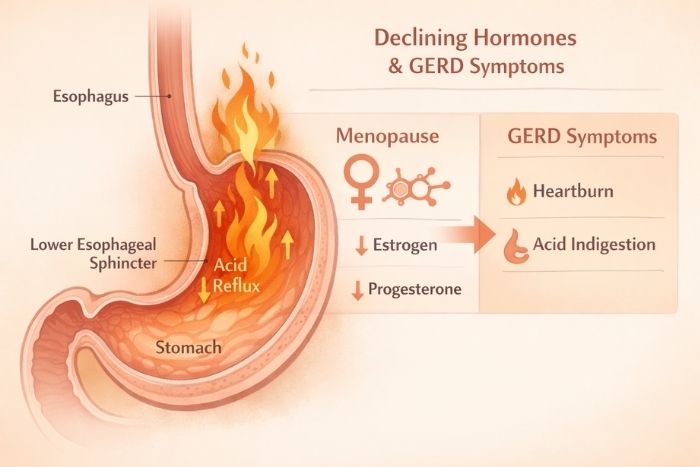
The Hormonal Mechanics of Reflux
You might be wondering what hormones have to do with stomach acid creeping up your esophagus. Turns out, quite a lot.
Progesterone’s protective role in maintaining the tone of your lower esophageal sphincter (the valve between your esophagus and stomach) becomes apparent when it declines[3]. This valve is supposed to stay closed except when you’re swallowing. When it weakens, acid can splash back up.
Additionally:
- Slower gastric emptying (another gift of declining hormones) means food and acid sit in your stomach longer
- Decreased muscle tone in the esophagus makes it less effective at pushing acid back down
- Changes in stomach acid production can create more irritation
- Increased abdominal pressure from bloating pushes stomach contents upward
I started experiencing reflux for the first time in my early 50s, and it was genuinely shocking. I’d never had heartburn in my life, and suddenly I’m sleeping propped up on pillows and avoiding tomatoes.
Taming the Fire Without Living on Antacids
Long-term antacid use isn’t the answer (though it might be necessary short-term). These medications can actually worsen gut health by reducing stomach acid needed for proper digestion and nutrient absorption.
Try these approaches first:
- Eat smaller, more frequent meals instead of three large ones. This reduces stomach pressure and acid production.
- Finish eating 3-4 hours before bed. I know this is tough, but it’s the single most effective change I made.
- Elevate the head of your bed by 6-8 inches. Gravity is your friend.
- Identify your trigger foods. Common culprits include coffee, alcohol, chocolate, tomatoes, citrus, and spicy foods. Yes, all the good stuff.
- Support stomach acid production naturally with apple cider vinegar in water before meals (start with 1 teaspoon) or digestive bitters. Bragg is the only one I use. It’s been a staple in my pantry for years.
- Manage stress because the gut-brain connection is real, and stress makes reflux worse.
When to see a doctor: If you’re experiencing reflux more than twice a week, having difficulty swallowing, or finding over-the-counter remedies ineffective, get evaluated. GERD can damage your esophagus over time.

Sign #5: The Unpredictability of It All (When Nothing Makes Sense Anymore)
This might be the most frustrating sign: the complete unpredictability of your digestive system.
One day you eat a salad and feel fine. The next day, the exact same salad leaves you bloated for hours. Last week, coffee was fine. This week, it triggers instant heartburn. Your bowel movements range from “finally!” to “seriously, again?” with no apparent pattern.
Welcome to the wild ride of digestive issues and menopause, where the rules change daily and your gut seems to have a mind of its own.
Why Consistency Becomes Impossible
The unpredictability stems from fluctuating hormone levels during menopause.
Your gut responds to these hormonal fluctuations in real-time:
- High estrogen days might mean more bloating and water retention
- Low estrogen days might trigger constipation and food sensitivities
- Progesterone spikes can slow digestion even further
- Stress hormones (cortisol) add another layer of chaos
It’s like trying to navigate a ship in constantly changing weather conditions. Just when you think you’ve figured out the pattern, everything shifts again.
Finding Stability in the Chaos
You can’t control your hormones’ wild ride, but you can create a foundation of gut support that helps regardless of what’s happening hormonally.
Build your stability plan:
- Establish non-negotiable daily rituals that support gut health: morning hydration, regular meal times, consistent sleep schedule, daily movement. Consistency in these areas creates stability when everything else is chaotic.
- Keep a “safe foods” list that you can rely on during flare-ups. Mine includes: baked/roasted sweet potatoes, cooked carrots, bone broth, chai seeds and baked chicken. Boring? Yes. Reliable? Absolutely.
- Practice stress management daily, not just when you’re overwhelmed. The gut-brain axis is particularly sensitive during menopause. Even 10 minutes of deep breathing or meditation helps.
- Supplement strategically with a quality probiotic, magnesium, and vitamin D. These support both gut health and hormonal balance.
- Give yourself grace. This isn’t a failure of willpower or discipline. This is your body navigating a major transition.
Track without obsessing. Use your journal to identify broad patterns rather than trying to control every variable. Look for themes like “worse during stressful weeks” or “better when I sleep 7+ hours” rather than “this exact food at this exact time.”

The Bigger Picture: You’re Not Broken, You’re Transitioning
Here’s what I wish someone had told me when my gut first started acting up during perimenopause: this isn’t a permanent state of dysfunction. It’s a transition.
Yes, it’s uncomfortable. Yes, it’s frustrating. Yes, it feels unfair that we have to deal with digestive chaos on top of hot flashes, mood swings, and all the other joys of menopause.
But understanding the gut-hormone connection gives us power.
When you know that your bloating is linked to declining estrogen affecting your microbiome diversity, you can take targeted action to support that microbiome. When you understand that slower gut motility is a hormonal issue, not a personal failing, you can implement strategies that actually address the root cause.
The 2025 research confirms what we’ve been experiencing: digestive issues and menopause are intimately connected, affecting the vast majority of us[1]. But it also reveals a critical gap: only 33% of women with digestive symptoms received a formal IBS diagnosis, and 55% reported significant impact on quality of life[1].
We’re suffering in large numbers, often without adequate support or even acknowledgment from healthcare providers.
That’s why we need to:
- Advocate for ourselves in medical appointments
- Seek practitioners who understand hormonal gut health
- Share our experiences with other women navigating this transition
- Implement bio-individual nutrition strategies that honor our unique needs
- Build community around these shared challenges
You’re not imagining your symptoms. You’re not being dramatic. And you’re definitely not alone.

Conclusion
The intersection of digestive issues and menopause affects an overwhelming majority of us: 94% according to the latest research[1]. Yet it remains frustratingly under-discussed and under-treated.
The five signs we’ve covered today: relentless bloating, stubborn constipation, new food sensitivities, unexpected reflux, and maddening unpredictability are all normal responses to the hormonal shifts happening in your body.
They’re not signs that you’re broken or doing something wrong. They’re evidence of the profound gut-hormone connection that science is only beginning to fully understand, particularly around the estrobolome and its role in metabolizing estrogen.
Your next steps:
- Start tracking your symptoms, foods, and patterns for at least two weeks. Data is power.
- Implement one change at a time from the strategies we’ve discussed. Don’t try to overhaul everything at once.
- Prioritize gut-supporting habits: hydration, movement, stress management, and sleep.
- Seek knowledgeable support from practitioners who understand the nuances of digestive issues and menopause.
- Join my community and explore more resources on navigating gut health during menopause.
Remember: This transition is temporary, but the self-knowledge and gut-health practices you develop now will serve you for decades to come.
Trial and error is okay. Giving up is not.
XOXO,



Ready to Fast-Track Your Relief?
If you’re feeling overwhelmed by where to start, or if your IBS and menopause bloating feel like they need a dedicated “intervention,” I’ve created something specifically for you.
I’ve taken everything I’ve learned from my own journey and the science behind Better Belly Co. to create “The Better Belly Reset: 7 Days to De-Bloat and Restart Your Digestion.“
Inside this FREE PLAN, I’ll show you:
- The exact 7-day meal plan designed to be gentle on the gut and high in bloat-busting minerals.
- The “Better Belly” List: A belly-friendly grocery guide focused on low-FODMAP, high-mineral foods.
- The “Gut-Hormone” morning ritual to kickstart motility before your first cup of coffee.
Click here to download The Better Belly Reset for free and let’s get you back to feeling like yourself again.
You’ve got this. We’ve got this. And I’ll be with you every step of the 7-day way.
Frequently Asked Questions:
Why did my bloating get worse during menopause?
Declining estrogen levels directly impact your gut microbiome by reducing bacterial diversity. This shift leads to increased gas production, reduced food breakdown, and higher water retention in your intestinal tract.
Can menopause cause new food sensitivities?
Yes. As estrogen declines, your body produces fewer digestive enzymes, making it harder to break down foods you once enjoyed. Changes in your microbiome, specifically the estrobolome, also create a feedback loop that increases sensitivity to triggers like dairy or high-FODMAP foods.
Is heartburn common in midlife?
It is very common. Nearly 49% of women in menopause report heartburn and acid reflux. This happens because declining progesterone affects the tone of the valve between your stomach and esophagus, allowing acid to creep up more easily.
How can I improve my gut motility naturally?
Focus on daily movement, like a 15-minute walk after meals, to stimulate your digestive tract. Strategic hydration, establishing a consistent morning routine with warm liquids, and prioritizing magnesium-rich foods can also help keep things moving.
Is there a link between IBS and menopause?
There is a strong connection. Research shows that 82% of women report their digestive symptoms started or worsened during the menopause transition. Hormonal fluctuations can turbocharge existing IBS-C symptoms, making consistency feel impossible.
References
[1] Digestive Health Issues More Common During Perimenopause And Menopause – https://menopause.org/press-releases/digestive-health-issues-more-common-during-perimenopause-and-menopause
[2] Understanding Perimenopause And Gut Health – https://cdhf.ca/en/understanding-perimenopause-and-gut-health/
[3] Menopause And The Gut – https://drstreicher.substack.com/p/menopause-and-the-gut
Note about Safety:
Note: These statements have not been evaluated by the FDA. These products are not intended to diagnose, treat, cure, or prevent any disease. Always consult your healthcare provider before starting any new supplement, especially if you have existing health conditions.

Jacqueline Ramirez
I help women in perimenopause and menopause navigate gut health with clarity and confidence. Through simple, gut‑safe food systems and real‑life guidance, I make eating feel calmer and more manageable again.






