Is Constipation a Symptom of Menopause? Why Digestion Changes After 40
You’re eating the same foods you’ve always eaten. You’re drinking your water. You’re doing everything “right.” And yet, your gut has completely changed the rules on you. 🙋♀️
If you’ve been wondering is constipation a symptom of menopause, the short answer is: absolutely yes. And you are far from alone. A major 2025 study of nearly 600 women found that 54% reported constipation during perimenopause or menopause and 82% said their digestive symptoms either started or got noticeably worse during this transition. [1]
I’m a woman in my 50s managing IBS-C and lactose intolerance during menopause. I know firsthand how menopause can feel like a double whammy on your gut. This article is my attempt to explain why this is happening and what we can actually do about it.
Key Takeaways 📌
- Yes, constipation is a recognized symptom of menopause. It’s not a coincidence, not in your head.
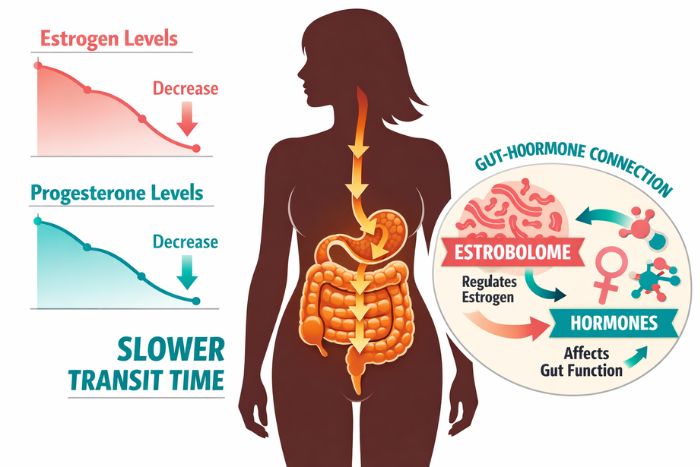
- Falling estrogen directly slows gut motility (how fast food moves through your digestive tract). [2]
- A specialized group of gut bacteria called the Estrobolome plays a huge role in your hormonal gut health.
- Stress and anxiety during menopause make constipation worse, sometimes more than hormones alone. [3]
- Simple, targeted changes to food, hydration, and daily habits can make a real difference.
So, Is Constipation a Symptom of Menopause? (Yes! Here’s the Proof)
Let’s put this question to rest for good.
A landmark study presented at The Menopause Society’s 2025 Annual Meeting looked at nearly 600 women aged 44–73. The results were eye-opening. A full 94% of perimenopausal and menopausal women experienced digestive health symptoms. [1]
Constipation came in as the second most common complaint, right behind bloating (77%). Stomach pain (50%) and acid reflux (49%) weren’t far behind. [1]
Here’s the part that really matters: 82% of women said these symptoms started or got worse specifically at perimenopause or menopause. [1] That’s not a coincidence. That’s biology.
💬 “Many women either don’t seek care or perceive their care as inadequate“, says Dr. Stephanie Faubion, Medical Director, The Menopause Society [1]
And yet, only 33% of women with these symptoms received a formal IBS diagnosis. [1] So if you’ve been suffering in silence, or felt dismissed by your doctor, you are not alone. We deserve better.
If you want a deeper dive into the bloating side of this equation, check out my article on why menopause bloating and IBS-C happen.
Why Menopause Slows Down Your Gut: The Hormone-Digestion Link

Here’s the core science explained without a medical degree required.
Estrogen and Gut Motility
Gut motility is just a fancy term for how fast things move through your digestive system. Think of it like traffic flow on a highway.
When estrogen levels are healthy, that highway moves smoothly. When estrogen drops, as it does during perimenopause and menopause, traffic slows to a crawl. Food and waste sit in your colon longer, water gets reabsorbed, and stools become hard and difficult to pass. [2]
That’s slower gut motility in a nutshell. And it explains why constipation during menopause feels so different from any constipation you’ve experienced before.
The Estrobolome: Your Gut’s Hidden Hormone Manager
This is the part most doctors don’t tell you about and it’s one of the most exciting areas of gut research in 2026.
The Estrobolome is a specific collection of gut bacteria that helps your body process and recycle estrogen. When your microbiome diversity is healthy, the Estrobolome works efficiently. When it’s disrupted, by stress, antibiotics, poor diet, or aging, estrogen metabolism goes haywire.
This creates a feedback loop: low estrogen disrupts gut bacteria → disrupted gut bacteria makes estrogen imbalance worse → worse estrogen balance slows your gut further.
It’s a cycle. And breaking it starts with understanding it.
Progesterone’s Role
Progesterone also drops during menopause. This hormone has a natural muscle-relaxing effect on the gut. Less progesterone = less smooth muscle movement = more sluggish digestion.
Postmenopausal women report significantly higher constipation rates than premenopausal women and this hormonal shift is a key reason why. [4]
How Constipation Makes Other Menopause Symptoms Worse
This is the part nobody talks about and it is worth the conversation.
Constipation during menopause doesn’t just cause discomfort on its own. It creates a ripple effect across your whole body.
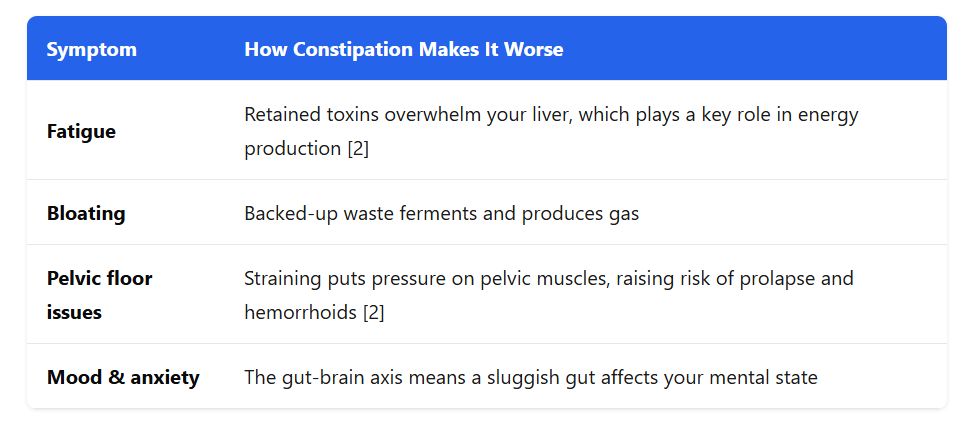
If you’re feeling exhausted on top of constipated, this connection is real. Your gut and your energy levels are deeply linked.
The Stress Factor: Why Anxiety Makes Midlife Digestive Flare-Ups Worse
Here’s something that surprised me when I first read the research.
Stress and anxiety are significant predictors of constipation severity during menopause, sometimes even more so than hormone levels alone. [3]
Menopause brings its own emotional weight: sleep disruption, mood swings, identity shifts. And all of that stress signals your nervous system to slow down digestion. It’s your body’s “fight or flight” response. Digestion is not a priority when your brain thinks you’re in danger.
The gut-hormone connection runs both ways. A stressed gut makes hormonal symptoms worse. Hormonal chaos stresses the gut.
What this means for us: Managing stress isn’t just self-care fluff. It’s a direct gut-health strategy.
What You Can Do: Practical Relief for Menopause-Related Constipation

Let’s get into the actionable part. Here’s what actually helps, based on both research and real life.
1. Prioritize Fiber (But Do It Slowly)
- Aim for 25–30g of fiber per day from whole foods
- Start slow: adding too much fiber too fast causes bloating
- Best sources: ground flaxseed, chia seeds, kiwi, pears, oats, leafy greens, legumes
- Ground flaxseed is my personal MVP: 1–2 tablespoons in a smoothie daily
2. Hydration Is Non-Negotiable
- Fiber without water is like trying to push a dry sponge through a pipe
- Aim for at least 8–10 cups of water daily
- Electrolytes help your body actually absorb that water, especially during menopause
- Check out my picks for the best electrolyte powders for women in menopause
3. Address Lactose Sensitivity in Menopause
Many of us develop new lactose sensitivity during menopause or find that existing intolerance gets significantly worse. Dairy can be a hidden driver of constipation and bloating.
- Swap cow’s milk for oat milk or almond milk
- Choose lactose-free options when dairy is unavoidable
- Watch for hidden dairy in protein powders and supplements
4. Try a Low-FODMAP Approach for Midlife
Low-FODMAP for midlife isn’t about restriction forever. It’s a short-term elimination tool to identify your personal trigger foods.
Common high-FODMAP culprits that worsen constipation and bloating:
- Onions and garlic
- Apples and pears (in large amounts)
- Wheat-based products
- Certain legumes
This is where bio-individual nutrition comes in. What works for your best friend may not work for you. Our guts are as unique as our fingerprints.
5. Support Your Microbiome Diversity
A diverse gut microbiome supports your Estrobolome, which, as we covered, is crucial for hormonal gut health.
- Add fermented foods: sauerkraut, kimchi (made without onion and garlic), kefir (dairy-free versions work great)
- Take a quality probiotic — see my guide to the best probiotics for bloating
- Eat the rainbow: different colored plants feed different gut bacteria
6. Move Your Body (Even Gently)
Exercise stimulates gut motility. You don’t need intense workouts.
- A 20–30 minute walk after meals can meaningfully improve transit time
- Gentle yoga, especially twisting poses, helps move things along
- Even light stretching beats sitting still
7. Try Gut-Healing Foods
Bone broth is one of my favorite tools for soothing an inflamed, sluggish gut. It’s rich in collagen and glycine, which support the gut lining.
Try my gut-healing bone broth recipe for women in menopause. It’s simple, nourishing, and genuinely helps.
How to Know If Your Constipation Is Menopause-Related

Use the Bristol Stool Scale as your quick reference guide. If your stools regularly look like Types 1 or 2 (small, hard, lumpy, or like separate pellets) that’s clinical constipation. [2]
Signs your constipation is likely menopause-related:
- It started or worsened around perimenopause (typically ages 45–55)
- It comes with bloating, gas, or acid reflux
- It’s worse during stressful periods
- Your diet hasn’t changed but your digestion has
When to see a doctor:
- Blood in stool
- Unexplained weight loss
- Constipation alternating with sudden diarrhea
- Symptoms that don’t respond to dietary changes after 4–6 weeks
For more on the gut-brain connection and navigating these changes, browse my Gut Feelings page. It’s one of my favorite places to send women who are just starting to connect the dots.
The Daily Routine That Helps Me Most
Here’s my honest, non-perfect daily approach:
- Morning: Warm lemon water before coffee
- Breakfast: Oatmeal with ground flaxseed and berries (dairy-free)
- Mid-morning: Electrolyte drink if I’m not hydrating well
- Movement: 20-minute walk, even if it’s just around the block
- Dinner: Cooked vegetables over raw (easier to digest for sensitive guts)
- Evening: Herbal tea (ginger or peppermint) and a wind-down routine to lower cortisol
Is it perfect every day? Absolutely not. But consistency over perfection is the whole game.
Conclusion: Your Gut Is Not Broken — It’s Changing
Is constipation a symptom of menopause? Yes and it’s one of the most common, most overlooked, and most treatable ones.
Your gut isn’t broken. It’s responding to a massive hormonal shift that affects everything from your Estrobolome to your stress response to how fast food moves through your system.
Here are your next steps:
- ✅ Track your symptoms for 2 weeks: note food, stress, and bowel patterns
- ✅ Add ground flaxseed and increase water intake this week
- ✅ Consider a dairy-free trial for 2 weeks if bloating is significant
- ✅ Explore a quality probiotic to support microbiome diversity
- ✅ Talk to your doctor if symptoms are severe or include red-flag signs
We’re in this together.


Ready to Fast-Track Your Relief?
If you’re feeling overwhelmed by where to start, or if your IBS and menopause bloating feel like they need a dedicated “intervention,” I’ve created something specifically for you.
I’ve taken everything I’ve learned from my own journey and the science behind Better Belly Co. to create “The Better Belly Reset: 7 Days to De-Bloat and Restart Your Digestion.“
Inside this FREE PLAN, I’ll show you:
- The exact 7-day meal plan designed to be gentle on the gut and high in bloat-busting minerals.
- The “Better Belly” List: A belly-friendly grocery guide focused on low-FODMAP, high-mineral foods.
- The “Gut-Hormone” morning ritual to kickstart motility before your first cup of coffee.
Click here to download The Better Belly Reset for free and let’s get you back to feeling like yourself again.
You’ve got this. We’ve got this. And I’ll be with you every step of the 7-day way.
Trial and error is okay. Giving up is not.
XOXO,

References
[1] Digestive Health Issues More Common During Perimenopause And Menopause – https://menopause.org/press-releases/digestive-health-issues-more-common-during-perimenopause-and-menopause
[2] 7 Menopause Symptoms Impacted By Constipation – https://www.avogel.co.uk/health/menopause/videos/7-menopause-symptoms-impacted-by-constipation/
[3] Pmc8080720 – https://pmc.ncbi.nlm.nih.gov/articles/PMC8080720/
[4] journals.sagepub – https://journals.sagepub.com/doi/10.1177/17455057251387470
Note about Safety:
Note: These statements have not been evaluated by the FDA. These products are not intended to diagnose, treat, cure, or prevent any disease. Always consult your healthcare provider before starting any new supplement, especially if you have existing health conditions.

Jacqueline Ramirez
I help women in perimenopause and menopause navigate gut health with clarity and confidence. Through simple, gut‑safe food systems and real‑life guidance, I make eating feel calmer and more manageable again.






