The Truth About Menopause Bloating: Why Real Food Beats Supplements Every Time
A staggering 94% of women report new or worsening digestive issues during perimenopause or menopause and bloating tops that list. [4] If you’ve been waking up with a relatively flat belly only to look very bloated by dinnertime, you are not imagining it. You are not broken. And you absolutely do not need a cabinet full of supplements to fix it.
I know firsthand how menopause bloating can feel like a cruel double whammy on top of gut issues you are already managing. So let’s skip the panic and get practical.

Key Takeaways
- Menopause bloating is driven by hormonal shifts specifically falling estrogen and progesterone, not a personal failure.
- Your gut microbiome changes during perimenopause, affecting how you digest food and process hormones.
- Real, whole foods outperform most supplements for sustainable perimenopause and menopause bloating relief.
- Slower gut motility (how fast food moves through you) is a root cause and diet can directly address it.
- Bio-individual nutrition matters; what works for your neighbor may not work for you, and that’s okay.
Why Menopause Bloating Is So Common (It’s Not Just You)
Nearly 77% of women aged 44–73 report bloating as a core menopause symptom. [4] In fact, research from the University of Washington found that 38% of postmenopausal women experience bloating, compared to just 14% of perimenopausal women. This means it often gets more intense as hormones settle at lower levels. [3]
So why does this happen?
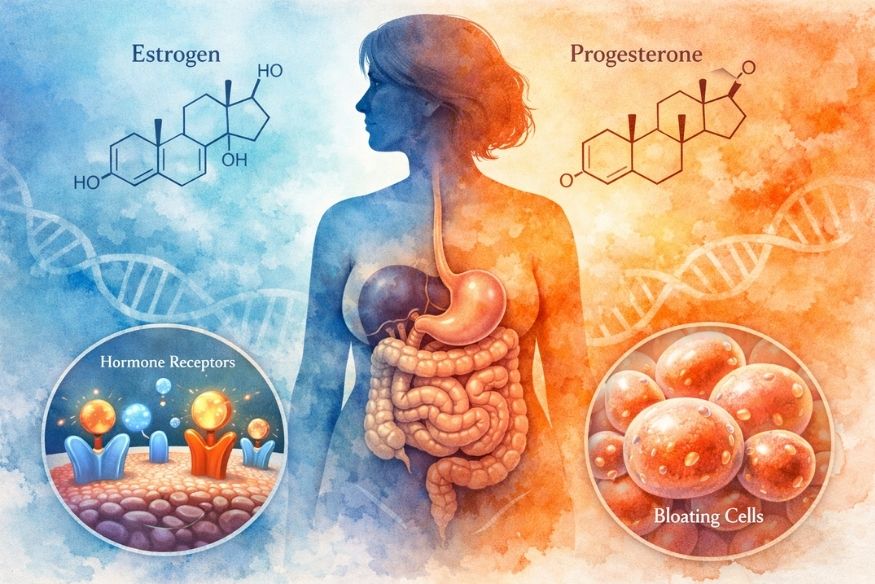
Estrogen and progesterone don’t just regulate your cycle. They regulate your entire digestive system. Estrogen receptors line your gut wall. When estrogen drops, those receptors become hypersensitive and you feel gas and pressure more acutely than you did at 35. [6]
Progesterone, meanwhile, is a natural muscle relaxant. Less progesterone means slower gut motility. Think of food moving through your digestive tract like a slow-moving traffic jam on a holiday weekend. Food sits longer. Gas builds. Bloating follows. [1]
There’s also a bile production piece. As estrogen declines, your liver produces less bile, the substance that breaks down fats. Less bile means fats are harder to digest, which creates more gas and discomfort. [5]
💡 The bloating you feel by evening isn’t a mystery. Gas and food accumulate throughout the day. By dinner, you’re stacking a new meal on top of everything that hasn’t fully moved through yet. [5]
For a deeper dive into the gut-hormone connection, check out my other articles featured in the section: gut health during menopause.
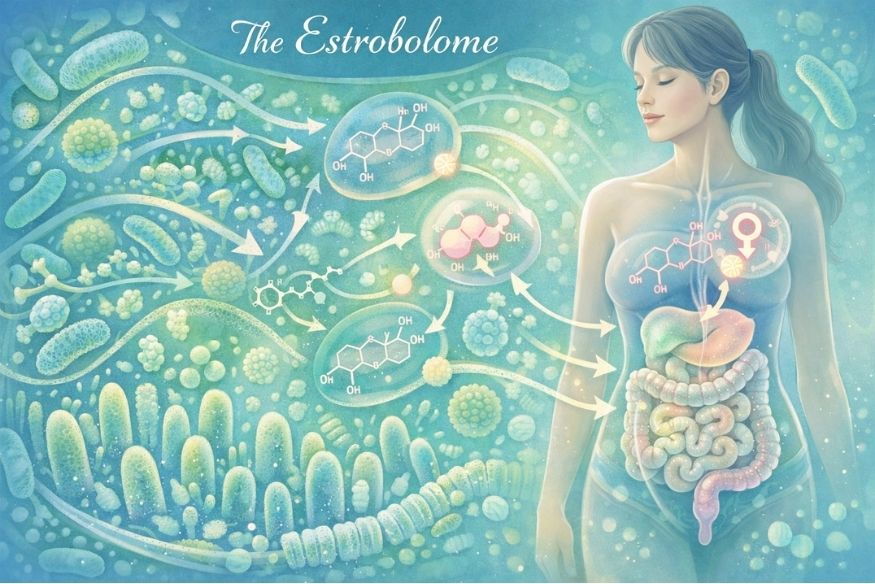
The Estrobolome: The Missing Piece Nobody Talks About
Here’s where it gets genuinely fascinating and where real food becomes your most powerful tool.
Meet the estrobolome: a specific collection of gut bacteria responsible for metabolizing and recycling estrogen. [1] When your estrobolome is healthy and diverse, it helps your body process estrogen efficiently. When it’s disrupted, by stress, antibiotics, a diet low in fiber, or just the hormonal chaos of perimenopause and menopause, estrogen metabolism goes sideways.
A disrupted estrobolome can worsen both hormonal imbalance and gut symptoms simultaneously. It’s a feedback loop that no single supplement can fully address.
This is why microbiome diversity matters so much in midlife. The more varied your gut bacteria, the better your body handles the estrogen fluctuations of this transition.
And here’s the kicker: you feed your estrobolome through food, not pills.
Fermented foods, prebiotic fiber, and polyphenol-rich plants are what these bacteria thrive on. No probiotic capsule, however well-formulated, can replicate the complexity of a diet rich in diverse whole foods.
That said, if you’re curious about whether a probiotic could support your protocol, I’ve done the research: see my guide to the best probiotics for menopause bloating.
Real Food Strategies That Actually Reduce Menopause Bloating
This is the heart of it. No dramatic elimination diet. No 30-day detox. Just smart, sustainable food choices that work with your changing body.
1. Build Your Plate Around Prebiotic Fiber
Prebiotic fiber feeds the good bacteria in your gut, including your estrobolome.
Best sources:
- Green bananas and slightly underripe plantains
- Cooked oats (resistant starch!)
- Garlic and onion (in small amounts if you’re sensitive or on a Low FODMAP diet)
- Leeks, asparagus, and artichokes
- Lentils and chickpeas (start small. More on this below)
Start low and go slow. Adding too much fiber too fast is a classic bloating trigger. Add one new high-fiber food per week.
2. Embrace Fermented Foods Daily
Fermented foods deliver live cultures and feed existing gut bacteria. They’re the real-food version of a probiotic.
- Sauerkraut (2 tablespoons with a meal is enough)
- Kimchi
- Dairy-free kefir (coconut or oat-based)
- Miso paste in soups and dressings
For a warming, gut-supportive meal, try my turmeric broth detox soup. It’s become a staple in my rotation.
3. Address Lactose Sensitivity in Menopause
This one is personal for me. Lactose sensitivity in menopause is extremely common, even in women who tolerated dairy fine for decades. Declining estrogen affects the production of lactase, the enzyme that breaks down lactose. [1]
If you’ve noticed dairy suddenly hitting differently, trust that instinct.
Simple swaps:
- Oat milk or almond milk for coffee and cooking
- Coconut yogurt for gut-friendly probiotics
- Nutritional yeast for a cheesy, savory flavor without the dairy
4. Try a Modified Low-FODMAP Approach
Low-FODMAP for midlife isn’t about eating boring food forever. It’s a short-term tool to identify your personal triggers.
FODMAPs are fermentable carbohydrates that feed gut bacteria, which sounds good, but if your gut is already inflamed and reactive, too many at once causes significant bloating.
Common high-FODMAP culprits during menopause:
- Apples, pears, and stone fruits
- Wheat-based products
- Garlic and onion in large quantities
- Beans and lentils (in large servings)
- Artificial sweeteners (sorbitol, mannitol, aspartame and saccharin)
The goal is a 2–6 week elimination phase, then systematic reintroduction. This is bio-individual nutrition in action. You learn your body’s map, not a generic one.
5. Cut the Gas Triggers (At Least Temporarily)
Some foods are reliable bloating triggers for most women during midlife digestive flare-ups. [2]
Reduce or temporarily eliminate:
- Carbonated drinks (yes, even sparkling water for some of us)
- Raw cruciferous vegetables in large amounts (broccoli, cauliflower, Brussels sprouts. Try them cooked instead)
- Chewing gum (you swallow air with every chew)
- Eating too fast (same issue: air swallowing)
Movement, Stress, and the Gut-Hormone Connection

Food is the foundation, but it doesn’t work in isolation.
Just 20 minutes of aerobic exercise three times per week can meaningfully reduce hormonal bloating. [2] A 10-minute walk after dinner is one of the simplest, most evidence-backed tools we have. [5] It stimulates gut motility, nudging that slow-moving digestive traffic jam along.
Stress is the other piece. Cortisol directly slows gut motility and increases gut sensitivity. [2] During menopause, when cortisol is already elevated due to hormonal disruption, chronic stress compounds every digestive symptom you’re already experiencing.
This isn’t about adding a meditation app to your to-do list. It’s about recognizing that rest is a gut health strategy.
A warm bath. Ten minutes of quiet. Saying no to one obligation. These aren’t luxuries. They’re medicine for your gut-hormone connection.
Also worth checking: are you getting enough electrolytes? Dehydration slows gut motility significantly. I’ve reviewed the best electrolytes for menopause bloating if you want a place to start.
Why Supplements Alone Will Always Fall Short

I want to be honest with you here, because I know how tempting the supplement aisle is when you’re desperate for relief.
Supplements can play a supporting role. I’m not anti-supplement. But no supplement can replicate the complexity of a diverse, whole-food diet.
Here’s why real food wins every time:

The supplement industry is worth billions precisely because it sells hope in a bottle. We deserve better than that.
If you want to explore what’s actually worth considering, my reviews of products for menopause cut through the noise with honest assessments.
A Simple Weekly Real-Food Gut Reset
You don’t need a complicated protocol. Here’s what one supportive week looks like:
Daily non-negotiables:
- ✅ 8+ glasses of water (add lemon or cucumber for variety)
- ✅ One serving of fermented food
- ✅ A 10-minute walk after your largest meal
- ✅ At least 25g of fiber from whole food sources
Weekly goals:
- 🥣 3+ different prebiotic foods
- 🥬 Cooked (not raw) cruciferous vegetables
- 🍲 One batch of gut-healing broth. My bone broth recipe for women in menopause is a reader favorite
- 🚶 3 sessions of 20-minute moderate movement
Reduce this week:
- Carbonated drinks
- Dairy (especially if you suspect lactose sensitivity)
- Artificial sweeteners
- Eating quickly while distracted
For more support on why menopause bloating and IBS-C happen together, I’ve written a full breakdown because understanding the why makes the what to do so much easier to commit to.
Conclusion: Work With Your Body, Not Against It
Menopause bloating is real, it’s common, and it’s rooted in genuine physiological change. This is not about willpower or discipline. This is about understanding that your body is navigating a major hormonal transition and supporting it with the most powerful tool available: food.
The estrobolome needs feeding. Your gut motility needs nudging. Your microbiome diversity needs tending. Real food does all three simultaneously, in a way no supplement stack can replicate.
Your next steps:
- Pick one fermented food to add to your meals this week.
- Swap one dairy product for a plant-based alternative and track how you feel.
- Add a 10-minute post-dinner walk to your daily routine.
- Reduce one known gas trigger, just one, for seven days.
- Explore my daily gut health routine builder to create a personalized plan.
Trial and error is okay. Giving up is not.
XOXO,



Ready to Fast-Track Your Relief?
If you’re feeling overwhelmed by where to start, or if your IBS and menopause bloating feel like they need a dedicated “intervention,” I’ve created something specifically for you.
I’ve taken everything I’ve learned from my own journey and the science behind Better Belly Co. to create “The Better Belly Reset: 7 Days to De-Bloat and Restart Your Digestion.“
Inside this FREE PLAN, I’ll show you:
- The exact 7-day meal plan designed to be gentle on the gut and high in bloat-busting minerals.
- The “Better Belly” List: A belly-friendly grocery guide focused on low-FODMAP, high-mineral foods.
- The “Gut-Hormone” morning ritual to kickstart motility before your first cup of coffee.
Click here to download The Better Belly Reset for free and let’s get you back to feeling like yourself again.
You’ve got this. We’ve got this. And I’ll be with you every step of the 7-day way.
FAQ:
Is it normal to suddenly become lactose intolerant during menopause?
Yes. Falling estrogen levels often reduce the production of lactase. This is the enzyme your body needs to break down dairy. Many women find that dairy products they enjoyed for years now cause gas and bloating. Switching to plant based milks or coconut yogurt often provides immediate relief.
Why does my bloating get worse in the evening?
Your digestive system slows down during menopause due to lower progesterone. This creates a traffic jam in your gut. As you eat throughout the day, food and gas accumulate because your motility cannot keep up. By dinner, you are adding new food on top of a system that has not finished processing breakfast or lunch.
Can I just take a probiotic pill instead of changing my diet?
Pills cannot replace the complexity of whole foods. Your estrobolome, the bacteria that manage estrogen, thrives on fiber and polyphenols found in plants. While some probiotics help, they work best when you feed your existing good bacteria with prebiotic foods like oats, leeks, and asparagus.
How long does it take for food changes to reduce bloating?
Most women notice a difference in comfort within two to six weeks. Your gut microbiome needs time to shift and adapt to new fiber levels or the removal of triggers like artificial sweeteners. Consistency with small daily habits matters more than a short term detox.
Does stress really impact how much I bloat?
Stress is a physical trigger for digestive issues. High cortisol levels slow down your gut motility and make your gut lining more sensitive to pressure. This means you feel gas and bloating more intensely when you are overwhelmed. Prioritizing rest is a practical way to support your digestion.
Should I stop eating raw vegetables?
Raw cruciferous vegetables like broccoli and cauliflower are very hard for a menopausal gut to break down. Cooking these vegetables softens the fibers and makes them easier to digest. If you love these foods, try steaming or roasting them instead of eating them raw in salads.
What is the fastest way to move gas through my system?
A ten minute walk after your largest meal is the most effective tool. Gentle movement stimulates the natural contractions of your intestines. This helps move food and trapped air through your system more quickly, which prevents the evening belly expansion.
References
[1] Menopause Bloating – https://www.forhers.com/blog/menopause-bloating
[2] Menopause Bloating – https://www.joinmidi.com/post/menopause-bloating
[3] Menopause Bloating – https://onlinemenopausecentre.com/menopause-bloating/
[4] Menopause Gas Bloat Indigestion – https://www.oprahdaily.com/life/health/a69488883/menopause-gas-bloat-indigestion/
[5] What Is Menopause Belly Why Do I Feel So Bloated – https://www.myalloy.com/blog/what-is-menopause-belly-why-do-i-feel-so-bloated
[6] Menopause Bloating Exp – https://www.weightwatchers.com/us/blog/menopause-bloating-exp
[7] Menopause And Bloating – https://us.onstella.com/menopause-symptoms/menopause-and-bloating/
[8] Perimenopause Bloating – https://www.oova.life/blog/perimenopause-bloating
Note about Safety:
Note: These statements have not been evaluated by the FDA. These products are not intended to diagnose, treat, cure, or prevent any disease. Always consult your healthcare provider before starting any new supplement, especially if you have existing health conditions.

Jacqueline Ramirez
I help women in perimenopause and menopause navigate gut health with clarity and confidence. Through simple, gut‑safe food systems and real‑life guidance, I make eating feel calmer and more manageable again.






